Introduction
Europe’s population is aging.
According to Eurostat, the percentage of people aged 80 or older in relation to the EU-27 population will increase two and a half times between 2019 and 2100, from 5.8% to 14.6%. Already now (2019 survey), more than one-fifth (20.3%) of the EU-27 population was at least 65 years old.
By the fact that the group of seniors is steadily growing, the voice for their needs is becoming increasingly important.
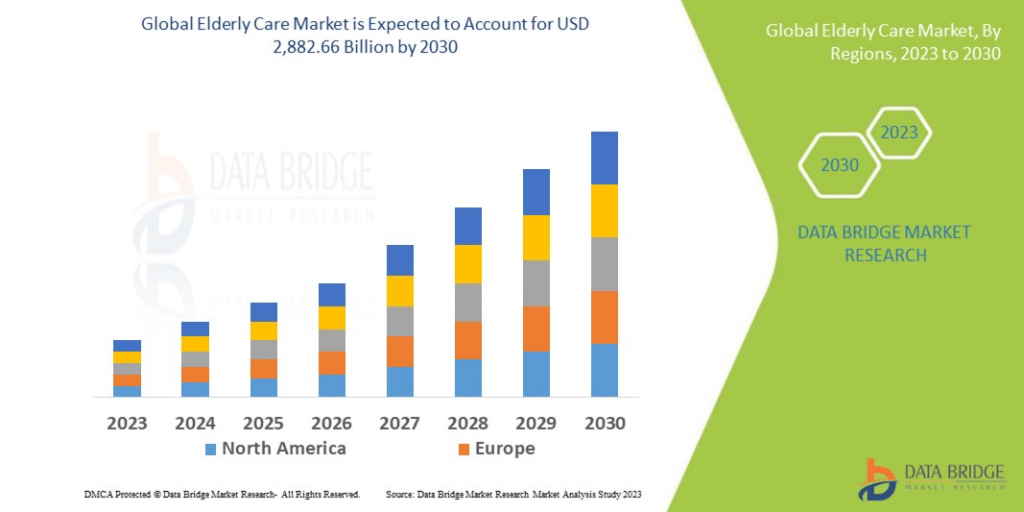
As a result, the value of the global senior care market is expected to be as high as $2,882.66 billion by 2030 (in 2022 the figure was $1,703.03 billion). The above growth is also influenced by the increasing incidence of chronic diseases in the elderly and the growing awareness of elderly care.
The primary need of this social group is health care. In a survey conducted in Poland by SeniorApp on a group of 352 seniors, when asked “what kind of help do you expect?” the highest-ranked answer (41.8%) was health care.
The healthcare sector therefore faces a challenge in how to respond to these needs. After all, many elderly people require regular medical contact or at least monitoring of basic health parameters. In an era of health sector staffing problems, solving the problem traditionally is not an option.
Therefore, the future of senior care is becoming telemedicine.
Telemedicine
Since the COVID-19 pandemic, telemedicine has been mainly associated with teleconsultations, i.e., talking to a doctor over the phone or the Internet, but the term itself is much broader. In addition to the aforementioned teleconsultations, in the context of senior care, one can additionally point to
- telediagnostics,
- telenursing,
- remote monitoring.
Each of these areas represents a separate service implemented with the help of integrated measurement devices.
Remote monitoring
The cornerstone of modern senior telehealth is remote monitoring.
A variety of devices are available on the market to monitor an elderly person’s condition in basic terms, that is, vital functions, location, or activity. More sophisticated devices can measure specific parameters such as blood saturation, ECG, blood pressure, glucose measurement, and the like.
These devices most often come in the form of a wristband or watch (they can also be special vests or so-called holsters), and in addition to monitoring functions, can initiate a call to a doctor or caregiver in an emergency. Also, to receive results from the devices, manufacturers offer smartphone or computer apps that make this possible.
With such functionalities, an elderly person in regular contact with his or her doctor does not need to physically appear at the clinic each time for routine checkups. Likewise, in the event of a sudden deterioration in well-being, the patient can immediately contact the doctor, who has real-time access to his or her health parameters. Monitoring can also apply to location – geofencing involves designating a safe zone (e.g., the closest area to the house) and, in the case of leaving it, notifying the caregiver.
All these functionalities significantly improve the quality of medical assistance offered to seniors and increase the comfort of care. They also affect the sense of security – knowing that in the event of an accident, someone will be immediately alerted to the fact, allows one to feel calmer.

Teleconsultations
The second pillar of remote senior care is teleconsultation. Of course, talking to a doctor remotely will never fully replace a physical visit, but it can be an important supplement to it, especially when it comes to the need to renew prescriptions for medications taken regularly or analyze test results. Teleconsultations allow seniors to quickly access medical specialists without having to leave their homes. Through video conferencing or even a simple phone call, an elderly person gains access to medical specialists regardless of where they live. This not only makes medical services more accessible to those with mobility difficulties but also eliminates the geographic barrier.
On the patient’s side, all that is needed for a teleconsultation is an ordinary phone or smartphone equipped with a camera, if a video connection is significant. It can also be a wristband or watch with such a function. The doctor, on the other hand, can also make the call from his phone or computer if his office system allows it.
Telediagnosis
Remote diagnosis involves making a diagnosis based on diagnostic tests, medical images, laboratory data, and other patient-related information sent online to the attending physician. In this case, the basis is medical records kept in electronic form, so that they can be exchanged between the facility performing the test and the diagnostician.
Thanks to telediagnosis, the patient is no longer responsible for bringing a physical copy of his test results and taking them to the appointment each time, since the doctor can access them in his system. For an elderly person, waiting to see a doctor with the results of their tests to get an opinion on them can be inconvenient and, in some situations, even dangerous. Nowadays, doctors can even issue an e-referral during a simple teleportation, which can be completed at the nearest facility performing the tests (and sometimes even at the patient’s home!). The results will be sent electronically to the doctor, so he or she can make a repeat diagnosis based on the latest data.
Doctors using telediagnostics also have access to clinical decision support tools, such as artificial intelligence algorithms. They can also support their clinical decisions with additional consultations with other specialists so that certain conditions can be detected at an earlier stage, which is of colossal importance for the elderly.
Telediagnostics has the potential to improve access to healthcare, especially for the elderly or patients living in remote regions with limited access to traditional medical care.
Telenursing
Telenursing, sometimes referred to as remote treatment plan management, refers to the use of technology to plan and manage patients’ health care. This approach can include the use of mobile apps, online platforms, or telephone communication to coordinate and plan health care without traditional visits.
For the elderly, they must be fully involved in their health maintenance plan. That’s why medical facilities provide their patients with apps or platforms that remind them to take their medications, perform routine tests, or exercise. Older patients can also manage their appointments, check their appointments, and so on.
These functionalities are important not only from the patient’s perspective but also for the operation of the clinic. Patients can manage their appointments without having to call the front desk. There is also the possibility to send him an SMS reminder for his next appointment, which can reduce the number of no-shows by up to 30%!
Conclusion
The new model of cooperation with the patient, not only in the elderly, assumes a greater role for telemedicine and its components: telediagnosis, teleconsultation, telenursing, or telemonitoring. The provision of medical services at a distance is becoming a new global trend, and healthcare leaders are investing in this area. According to the Philips Future Health Index 2023 report, more than two-thirds (68%) of Polish healthcare leaders and young medical professionals believe that virtual care is the technology that has or will have the greatest impact on improving patient care.
This trend is particularly evident among aging societies such as Poland. Although the National Health Fund does not reimburse telemonitoring devices at this point, some local governments are setting aside funds for the purchase of life bracelets as part of their social care funds and are distributing the devices free of charge.
This is a step in the right direction, improving the comfort of life not only for seniors but also for their families.
Modern telemedicine solutions, combined with the e-services made available by the e-Health Center, make it safe to say that this is the beginning of the end of the traditional model of medical care, which in the case of providing these services to seniors means greater ease and accessibility.
Sources:
- https://www.databridgemarketresearch.com/reports/global-elderly-care-market
- https://ec.europa.eu/eurostat/statistics-explained/index.php?title=Archive:Struktura_ludno%C5%9Bci_i_starzenie_si%C4%99_spo%C5%82ecze%C5%84stwa
- https://seniorhub.pl/wp-content/uploads/2021/12/SeniorApp_Raport_2021.pdf
- https://samorzad.pap.pl/kategoria/jak-robia-inni/w-lodzi-500-seniorow-otrzyma-opaski-bezpieczenstwa